How a rural hospital strengthened financial performance through improved charge capture
Rural hospitals across the United States continue to face increasing financial pressure. Declining reimbursement rates, rising operational costs, workforce shortages, and limited access to specialized resources all contribute to narrowing margins. In this environment, ensuring hospitals are accurately capturing and billing for the care they already provide is essential to long-term sustainability.
Johnson Memorial Hospital in Franklin, Ind., reflects many challenges common among rural health care organizations. Like many of its peers, the hospital faced difficulties capturing all eligible charges in its operating room and emergency department, which led to missed reimbursement opportunities. Addressing these gaps became a priority as margins tightened and operational efficiency grew more critical.
Common challenges in rural charge capture
Charge capture issues in rural hospitals often stem from a combination of operational and structural factors. Limited staffing can create documentation gaps, while complex coding and reimbursement rules make it difficult to ensure every billable service is captured accurately. Additionally, rural hospitals frequently lack the internal resources or specialized expertise to conduct comprehensive revenue audits.
To address these challenges, many rural hospitals turn to external consultants. While consulting engagements can provide valuable insights, they may also require significant internal effort to implement recommendations. In some cases, the cost and complexity of traditional consulting models limit their overall effectiveness for resource-constrained organizations.
Case study overview: Johnson Memorial Hospital
Recognizing that missed charges were contributing to revenue leakage, leadership at Johnson Memorial Hospital sought an approach that would improve charge capture without placing additional strain on staff or requiring major system changes. The hospital elected to partner with Net Revenue, a Hudson, Ohio-based firm that focuses on improving reimbursement in operating rooms and emergency departments through enhanced charge capture and cost analysis.
Dr. David Dunkle, president and CEO of Johnson Memorial, noted that the decision was driven by a fundamental challenge facing many rural hospitals: “We were simply not getting paid properly for the services we provided, and with margins continuing to decrease, we needed to ensure we were reimbursed accurately for the care we deliver.”
 Dr. David Dunkle
Dr. David Dunkle
Establishing a data-driven audit process
A foundational step in improving charge capture is conducting a thorough audit. At Johnson Memorial, the assessment process was designed to minimize disruption and limit the need for internal IT resources. Required data was straightforward and focused on claims and charge information already available within existing systems.
Once the data was collected, a clinical audit team reviewed claims to identify patterns of underbilling, missed charges, and documentation gaps. This review examined how services were recorded, coded, and ultimately billed, with close attention to areas that commonly present challenges in rural hospital settings.
After completing the audit, findings and recommendations were shared with hospital leadership to establish agreement on the scope of improvement efforts before moving forward.
Key steps to improving charge capture in OR and ER settings
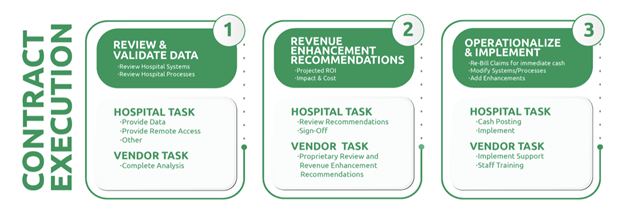
Based on the assessment process, several core steps emerged as essential to improving charge capture in rural hospitals:
- Gather and validate data
Ensure that charge and claims data is complete, accurate, and representative of current operations. - Conduct a comprehensive audit
Review claims in detail to identify missed charges, inconsistencies, and process breakdowns that affect reimbursement. - Align documentation and charging processes
Organize charge workflows in a way that reflects clinical practice and supports accurate billing. - Implement follow-up and recovery measures
Act on identified opportunities by submitting appropriate follow-ups and recovering missed revenue where permissible. - Educate staff and establish ongoing oversight
Provide guidance and tools that support sustained improvement beyond the initial audit period.
Following these steps helps rural hospitals increase the likelihood of capturing eligible charges while building processes that support long-term financial performance.
Measurable results from the operating room review
At Johnson Memorial, the scope of the audit included more than 1,000 operating room claims, along with a detailed review of charging practices. The assessment revealed multiple opportunities to recover reimbursement for services that had already been provided but were not fully captured.
As a result of the OR initiative, Johnson Memorial generated more than $2 million in annual reimbursement. Notably, this outcome was achieved with ongoing support required from hospital staff, allowing teams to remain focused on providing patient care and daily operations.
Expanding improvements to the emergency department
Following the success of the operating room review, Johnson Memorial expanded the scope of the initiative to include its emergency department. Emergency departments often present unique charge capture challenges due to high patient volume, variable acuity levels, and fast-paced clinical workflows.
The emergency department audit included approximately 2,500 claims and total charges exceeding $30 million across both OR and ED services. Applying the same structured review and recovery process allowed the hospital to identify additional reimbursement opportunities without introducing new administrative burdens.
Financial impact across OR and ER services
Through the combined operating room and emergency department initiatives, Johnson Memorial recovered more than $5 million in reimbursement for work that had already been completed. The emergency department expansion alone contributed an additional $3.5 million in recovered revenue.
These results demonstrated how targeted, data-driven charge capture improvements can significantly strengthen financial performance for rural hospitals when implemented thoughtfully and efficiently.
Supporting long-term sustainability through education
Beyond the immediate financial outcomes, the initiative emphasized sustainability through staff education and process improvement. Rather than limiting engagement to a one-time assessment, the approach included guidance designed to help hospital teams understand charge capture risks and maintain improved practices over time.
Reflecting on the experience, Dunkle highlights the importance of this focus on continuity: “They educated our staff and provided us with a game plan for success long after the initial work was completed.”
Many organizations consider an engagement successful once recommendations are delivered. In this case, the emphasis on execution, education, and follow-up helped ensure that improvements extended beyond short-term recovery.
Lessons for rural health care leaders
Johnson Memorial Hospital’s experience illustrates several key lessons for rural health care leaders:
- Missed charge capture can represent a significant but addressable source of lost revenue.
- Data-driven audits can be conducted with minimal internal disruption.
- Sustainable improvement depends on both recovery efforts and staff education.
- Periodic reviews can help ensure continued accuracy as workflows and regulations evolve.
By focusing on practical solutions that align with existing resources, rural hospitals can strengthen financial performance while continuing to prioritize patient care.
NRHA adapted the above piece from Net Revenue, a trusted NRHA partner, for publication within the Association’s Rural Health Voices blog.
 | Chris Milligan is the chief revenue officer for Net Revenue. He has over 30 years of experience in all aspects of the revenue cycle process and has earned his MBA from Ashland University and received his CRCR and CHFP certifications through the Healthcare Financial Management Association. |
